Novel Materials for Regenerative Wound Healing
Wound healing and scar reduction are important goals of wound therapies which can now be achieved by novel regeneration promoting materials
Research published online in Advanced Healthcare Materials in March, 2023
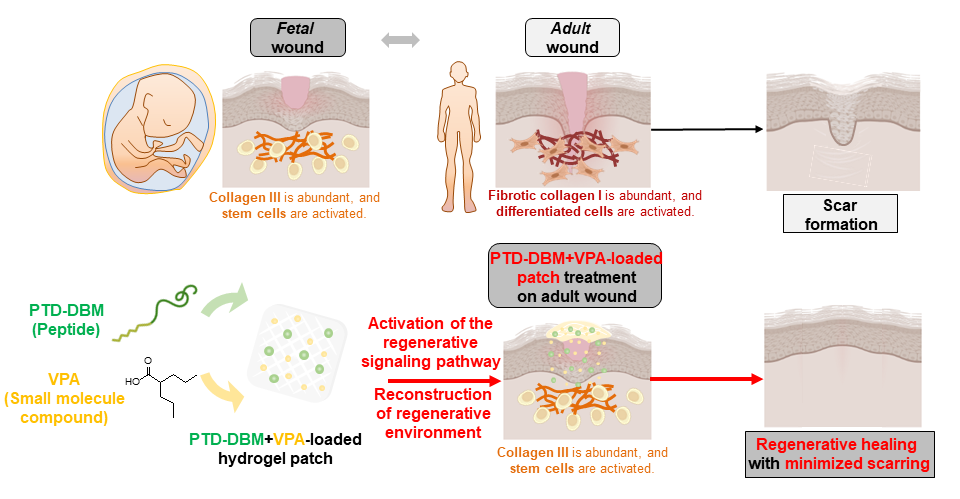
Photo credits: Dr. Kang-Yell Choi, Yonsei University
During wound healing, human fetal skin develops normal, scar-free skin tissue after injury. This phenomenon, called regenerative healing, is enabled by the abundance of stem cells and the protein Collagen III. However, adult human skin does not undergo regenerative healing, which results in scarring. Triggering the regenerative healing pathways in adult humans could minimize scarring during wound healing, which can improve the quality of life for patients suffering from various types of wounds.
According to a research article in Advanced Healthcare Materials, a team of scientists led by Dr. Kang-Yell Choi at the Yonsei University in Korea have devised a novel patch for delivery of pro-regenerative material that can promote regenerative wound healing in mice. This patch could act as a potential therapeutic agent for wound healing and scar reduction in different kinds of acute and minor wounds. It may also find applications in the treatment of chronic wounds like bedsores or diabetic foot ulcers.
“We developed and used a pyrogallol-functionalized hyaluronic acid (HA-PG) patch as a drug delivery system for local and sustained delivery of pro-regenerative materials to the wounds.” says Dr. Choi. Hyaluronic acid is known to promote cellular movement and trap water, aiding regeneration in human fetuses. The high affinity of the pyrogallol molecule for multiple substrates allows the simultaneously delivery of multiple materials that work synergistically.
In mouse models, the HA-PG patch showed clear self-crosslinking abilities and excellent tissue-adhesiveness. The HA-PG patch could effectively deliver a combination of two substances: protein transduction domain-fused Dishevelled-binding motif (PTD-DBM) and valproic acid (VPA). Both of these are known to promote wound healing in mice by activating the regenerative Wnt/?-catenin signaling pathway.
The HA-PG patches with PTD-DBM and/or VPA brought about an increase in the expression of stem cells at the wound site. They achieved this through the suppression of differentiated cell markers and promotion of stem cell markers in the cells at the wound site. The production of Collagen III, which is associated with scarless wound healing, was also noted. As Dr. Choi mentions, “Collectively, these data show that the HA-PG patches with PTD-DBM and/or VPA not only promote cutaneous wound healing but also inhibit scar formation.”
Thus, treatment with HA-PG patches loaded with PTD-DBM and/or VPA not only promotes wound healing, but also produces Collagen III which is an important factor for scarless regenerative healing. There are no reported adverse effects of long-term treatment with PTD-DBM on the skin, making this a safe treatment option. The pro-regenerative materials targeting the regenerative signaling pathway could be highly beneficial for the treatment of many patients by inducing regeneration in various damaged tissues, including skin wounds.
Recommended Articles
Professor Jong-Hyun Ahn
Novel technique for producing high-resolution micro-LED displays
Professor Seong Chan Jun
Professor Donghyun Kim
Array of hope: Up close and personal with mitochondria in neurons