Catch It Early, Save a Mind: Fluid Markers Can Help in the Early Detection of Alzheimer’s
Alzheimer’s disease (AD) is the most common cause of mental decline in the elderly. Its symptoms range from mild cognitive impairments to a serious decline in memory, communication, and behavior. The treatment of AD has remained challenging over the years, especially because symptoms do not appear until the disease reaches its advanced stage. This makes you wonder: is there a way to diagnose AD before the start of its debilitating symptoms? In an insightful review published in Experimental & Molecular Medicine, researchers at the Yonsei University, led by Dr YoungSoo Kim, dig deeper into ways to detect AD.
AD is linked mainly to the misfolding of two proteins: amyloid beta and tau. Fragments of these proteins clump together in the brain, forming plaques and tangles in brain cells and subsequently leading to cognitive damage. In AD, these fragments are seen to be present in the fluid around the brain and the spinal cord (called the “cerebrospinal fluid”), as well as in fluids of the eyes, nose, mouth, and blood. Thus, these proteins can serve as “fluid biomarkers” for the detection of AD.
In their review, the scientists discuss the capabilities and limitations of using these fluid biomarkers as diagnostic tools for AD. They based their research on a previous study by the team, published last year in Science Advances, in which they had successfully diagnosed 93% of patients with AD using plasma biomarkers. In this review, to begin with, they compare the different sources from which these fluid biomarkers can be obtained. They note that biomarkers in the cerebrospinal fluid are the most effective in diagnosing AD at an early stage. However, obtaining these samples is expensive and uncomfortable for patients. Moreover, they point out that data on the effectiveness of fluid markers from blood and other sources are currently limited. But on the bright side, they offer various benefits: they are easy to obtain and inexpensive owing to their accessibility. Thus, further research is needed to fine-tune the utility of blood-based biomarkers for the diagnosis of AD. Similarly, although oral, retinal, and ocular fluids are easy to obtain, their sensitivity as diagnostic tools is debated. Thus, further research might help to clarify the use of these fluids as diagnostic markers in AD.
The researchers go on to explain that current diagnosis of AD relies on the visualization of brain damage, but by the time any damage is apparent, it is likely that the disease has reached an advanced stage. Thus, a combination of visualization techniques and assessment of fluid biomarkers would enable the early detection of AD in asymptomatic patients. The authors also summarize the progress made over the years in establishing the latest guidelines for AD diagnosis through an elegant figure (Figure 1). Dr Kim explains, “In our review, we consider how the amyloid beta and tau biomarkers from different sources can be used in clinical settings.”
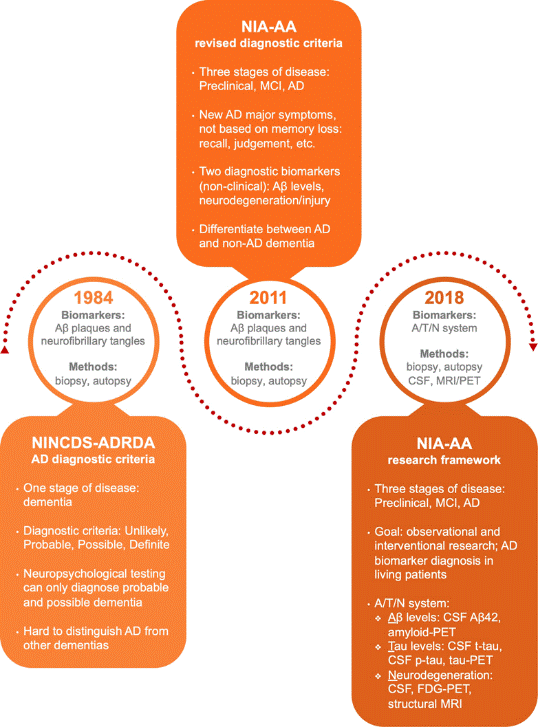 Figure 1. A timeline of revisions applied to the protocols for AD diagnosis. The AD diagnostic criteria have reflected the expansion of understanding of AD pathology. The clinical diagnostic underwent two major revisions after its initial publication in 1984 - the latest revision occurred in 2018
Figure 1. A timeline of revisions applied to the protocols for AD diagnosis. The AD diagnostic criteria have reflected the expansion of understanding of AD pathology. The clinical diagnostic underwent two major revisions after its initial publication in 1984 - the latest revision occurred in 2018
(photo credits: Experimental & Molecular Medicine)
In AD, cognitive decline and the accompanying loss of independence puts a huge burden on patients and their caregivers. This study paves the way for the development of inexpensive and accessible fluid markers for the early diagnosis of AD. Owing to these comprehensive findings, this review was selected to be part of the “Springer Nature 2019 Research Highlights.” Dr Kim is optimistic about the implications of the study. He says, “I believe that our study will be useful in the development of novel diagnostic tests for AD. The hope is to ultimately reduce the negative impact of AD on the elderly community.”
updated in May 2020
Recommended Articles
Professor Hyuk-Jae Chang
Professor Sung-Joo Hwang